When I hear the phrase “integral human development,” the picture that comes to mind is a developing fetus—the beginning of human development. Human development begins with the conception, gestation, and birth of a baby, which we tend to think of as a joyous moment worth celebrating.
To a pregnant mother, the birth of her baby is the culmination of a “forty-week” journey marked by numerous bodily changes, emotional swings, and other challenges. Although the journey from pregnancy to childbirth can be difficult, we often tell pregnant women, using an all-too-common phrase, that “you will soon have your bundle of joy.” Many pregnant women look forward with anxious anticipation to the birth, imagining baby snuggles and all of the beauty they will witness in and through their child.
Many pregnant women around the world are deprived of the opportunity, however, to watch their baby grow and become an integral part of society. For them, pregnancy and childbirth arouse mixed emotions. This is particularly true for women who have been deprived of their rightful access to maternal health care. The joy in anticipating their baby’s arrival is tempered with the dread of the real possibility of sacrificing their lives in the process. The “joy of childbirth,” for many women and their families, is complicated and overshadowed by the “fear of childbirth.”
“A deep, dark continuous stream of mortality . . . how long is this sacrifice to go on?”This cry of concern was voiced in 1838 by William Farr, the first registrar general of England and Wales. Although women have been dying since time immemorial from preventable causes related to pregnancy and childbirth, it wasn’t until 1987 that a global initiative was launched to reduce the number of preventable maternal deaths: the safe motherhood initiative.
A mother’s right to life
Why did it take so long for a mother’s right to life to become a priority on the global development agenda? Over three decades later, too many women are still sacrificing their lives each day to give life. The question remains: “how long will this sacrifice linger?”
Maternal mortality, defined by the World Health Organization (WHO) as the death of a woman while pregnant or within forty-two days of the end of pregnancy, is a critical global health challenge. It is unacceptably high, particularly in developing countries. Although there was a 38 percent reduction in the global maternal mortality ratio between 2000 and 2017, the WHO estimates that around the world, a jaw-dropping 810 women die every single day due to complications of pregnancy and childbirth. Nearly 94 percent of these deaths occur in low and lower-middle income countries, and the vast majority of these deaths (two-thirds) occur in sub-Saharan African countries, making it the region with the greatest maternal mortality burden.
Sadly, the United States is not immune from this preventable tragedy. Estimates from the WHO indicate that the US maternal mortality ratio (MMR) is nineteen maternal deaths for every 100,000 live births, compared to the average of eleven deaths per 100,000 live births for all other high-income countries. For comparison, the MMR for every 100,000 live births is two in Norway, four in Spain and Sweden, five in Belgium and Netherlands, six in Australia, seven in the United Kingdom and Germany, eight in France, and ten in Canada.
Even more troubling, while maternal mortality ratios are generally decreasing globally, the US has been heading in the opposite direction with increasing maternal mortality. Maternal deaths here in our university’s own state of Indiana, for example, have been consistently higher than the US national average for several years.
Racial inequities
Further, there is compelling evidence that racial inequities play a significant role in America’s maternal mortality burden. Black women are more than three times more likely than White women and Hispanic women to die during pregnancy, childbirth, and the postpartum period. A google search of Black maternal mortality will bring up several stories that indicate that the inequities Black mothers face in maternal deaths extend beyond pre-existing educational and socioeconomic inequities that contribute to poorer access to care.
Institutional racism across many levels of America’s health care system plays a significant role in the Black maternal death crisis. From the death of Kira Johnson in 2016 to the death of Shalon Irving in 2017, there are numerous cases of Black mothers dying in the United States from preventable causes, much like in less developed countries.
Global initiatives
The United Nations’ Sustainable Development Goal 3 of “ensuring healthy lives and promoting well-being at all ages” provides a number of key global health targets. The first is to decrease the global maternal mortality ratio from 211 to below seventy maternal deaths per 100,000 live births by 2030. In addition, no individual country should have a maternal mortality ratio more than twice the global average.
For many countries in Sub-Saharan Africa, achieving this goal by 2030 is far-fetched. Socioeconomic and cultural factors, poor access to health care facilities, and poor quality of care remain significant obstacles to maternity care in the region. As the global community strives to decrease preventable maternal deaths, interventions, programs, and policies must target women who are most vulnerable to this scourge of maternal mortality.
Historically, global initiatives, programs and interventions for mothers and babies have been combined (maternal/newborn health or maternal/child health interventions). This makes sense during pregnancy, because the mother carries the fetus and her health affects the baby’s health. It also makes sense immediately after birth, because the mother is the primary caregiver of the newborn, and in many cases, the primary source for their infant’s nutritional needs.
While this combined mother-baby approach is well-intentioned, more often than not it prioritizes the baby’s health over the mother’s health. In Maternal Mortality–A Neglected Tragedy: Where is the M in MCH?, a 1985 article published in the Lancet, Rosenfield and Maine drew attention to the fact that causes of maternal deaths are different from those of infant mortality, and therefore should merit unique interventions. They called on global actors like the World Bank to make maternity care one of its priorities. In a major step forward, the Millennium Development Goals, specifically Goal 5A, and, now, the Sustainable Development Goal 3.1, specifically targets maternal deaths.
Neglect of the mother’s health is seen especially after birth or the postpartum period, when postnatal care of the baby becomes more important than postpartum care of the mother. I would argue that the neglect of quality postpartum care of the mother is a major contributing factor to high maternal death rates. In the design of integrated Maternal/Newborn Health (MNH) or Maternal Child Health (MCH) programs and interventions, particularly in the postpartum period, the “M” in MCH or MNH should not be forgotten: postnatal care of the baby without postpartum care of the mother is a job half done!
Current research
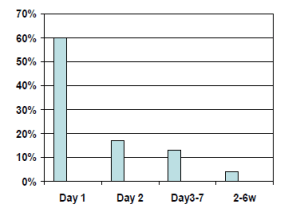
My research is dedicated to improving maternal health outcomes during the postpartum period, the timeframe when mothers are at highest risk for maternal deaths. Specifically, I examine patient and healthcare facility factors that influence access to quality postpartum care among vulnerable populations in Sub-Saharan Africa and the United States. In many settings in Sub-Saharan Africa, quality postpartum care, education, and support for the mother are often missing components in postnatal care, which focuses on care of the baby. In Malawi, I examined whether women who delivered in health facilities received the recommended postpartum clinical assessments before discharge, and found that although women delivered in health facilities with skilled birth attendants, most were not examined after delivery. I have also assessed midwives’ knowledge of postpartum care and complications among 245 midwives in four hospitals in Tamale and found significant knowledge gaps in care of the postpartum patient and recognition of warning signs of life-threatening complications.
I am currently working to improve postpartum care and education of mothers by implementing and evaluating an intervention known as Focused-PPC in four health centers in Tamale, Ghana. Focused-PPC is an innovative postpartum care, education and support model that integrates recommended clinical care for mother and baby, and includes education and support for mothers in a group setting for up to twelve months after birth. Each group will meet at one-to-two weeks, six weeks, and monthly thereafter for up to one year postpartum following the Ghana Health Service postnatal care schedule. Led by trained midwives in the health centers, each group session will consist of postpartum clinical assessments for mother (in addition to baby), education, and support. Our model will ensure that mothers receive quality postpartum care and education as recommended by the World Health Organization and Ghana Health Service.
Every woman should have the right to quality maternity care services, regardless of where they live or give birth. Mothers are integral to human development. The impact of maternal deaths has lifelong consequences for their babies, older children, families, and the community at large.
Let us persist in our quest to ensure healthy lives for all human beings, including the lives that give life.
Previously Published by the author in Dignity & Development, a series of blog posts by the Keough School of Global Affairs, University of Notre Dame, that provides in-depth analysis of global challenges through the lens of integral human development.





 receive in health facilities after delivery. Husbands who are aware of some of these services get the information from their wives. Also, many husbands do not usually attend postpartum care visits with their wives. Even for husbands who accompany their wives for care, they seldom enter the health facility.
receive in health facilities after delivery. Husbands who are aware of some of these services get the information from their wives. Also, many husbands do not usually attend postpartum care visits with their wives. Even for husbands who accompany their wives for care, they seldom enter the health facility.





 On Monday, August 27th, I announced to my parents and other people about my new program, and right after making all those calls (no kidding), I got an unexpected call from the University of Iowa Hospital for an interview! I had given up waiting for that call…and then it came. I was scheduled for an interview on August 31, and I went for it. Why did I go? … well, that was my original plan … before the whole PhD craziness started. Judith and I had thought we would be roommates when I got the job. She was in dental school in Iowa. It was a great interview, and they told me to expect a call in two weeks. Meanwhile, on the MSU side of things, I got an email that the admissions office needed an affidavit of $$$$$; let’s just say a ton of money to prove that I could afford tuition before they could process the admission. Once again, I needed to show proof of finances for the tuition before an I-20 (important document International students must have) could be processed. I had to tell yet another school that I did not have money. But this time around, things worked out! The college of nursing gave some funding on admission, and I was able to apply for and obtain a graduate assistantship within the college.
On Monday, August 27th, I announced to my parents and other people about my new program, and right after making all those calls (no kidding), I got an unexpected call from the University of Iowa Hospital for an interview! I had given up waiting for that call…and then it came. I was scheduled for an interview on August 31, and I went for it. Why did I go? … well, that was my original plan … before the whole PhD craziness started. Judith and I had thought we would be roommates when I got the job. She was in dental school in Iowa. It was a great interview, and they told me to expect a call in two weeks. Meanwhile, on the MSU side of things, I got an email that the admissions office needed an affidavit of $$$$$; let’s just say a ton of money to prove that I could afford tuition before they could process the admission. Once again, I needed to show proof of finances for the tuition before an I-20 (important document International students must have) could be processed. I had to tell yet another school that I did not have money. But this time around, things worked out! The college of nursing gave some funding on admission, and I was able to apply for and obtain a graduate assistantship within the college.
